Blood pressure readings from a single clinic visit can be misleading for an accurate hypertension diagnosis. If you’ve ever left a clinic thinking, “That number can’t be right,” you’re not alone.
Ambulatory blood pressure monitoring (often shortened to ABPM) helps solve that problem by tracking your blood pressure over a full day and night, while you live your normal life. It’s one of the best ways to confirm whether you truly have high blood pressure, and it can also show patterns that a clinic cuff can’t see.
What ambulatory blood pressure monitoring is (and why it’s so helpful)
ABPM is a non-invasive test where you wear an automatic blood pressure cuff for about 24 hours. The cuff inflates at intervals during the day and while you sleep, often utilizing the oscillometric technique to take measurements. Those repeated readings build a real-world picture of what your blood pressure does at work, on errands, during stress, and at rest.
That matters because office blood pressure readings can mislead in both directions:
- White coat hypertension: your blood pressure rises in the clinic because you feel tense.
- Masked hypertension: your clinic number looks fine, but your blood pressure runs high at home.
ABPM can catch both, which is why many experts treat it as the gold standard for diagnosis. If you want the medical deep dive, the review titled ambulatory blood pressure monitoring in arterial hypertension explains why out-of-office blood pressure measurements often predict risk better than a one-time office number.
What it feels like to wear an ABPM device for 24 hours
Most people get fitted in a clinic, then go on with their day. The cuff is on your upper arm and connects to a small blood pressure monitor that clips to your belt or sits in a pouch, tracking systolic blood pressure and diastolic blood pressure throughout the 24-hour period. When it inflates, it can feel tight, especially if you’re mid-task. Still, the discomfort is brief.
A few simple habits can make the day smoother:
Keep living normally, because “normal” is the point. At the same time, when the cuff starts to inflate, pause your movement, keep your arm relaxed, and avoid talking until it finishes. That mirrors good measurement habits recommended for accurate readings in general, including heart rate recorded by the device.
Nighttime can be the strangest part. The cuff may wake you once or twice. Even so, those sleep readings are valuable because they reveal patterns like nocturnal dipping, where blood pressure normally falls in alignment with the body’s circadian rhythm. Some people’s blood pressure stays high at night, missing this dip, which can raise long-term heart risk.
How to understand an ABPM report (without getting lost in the details)
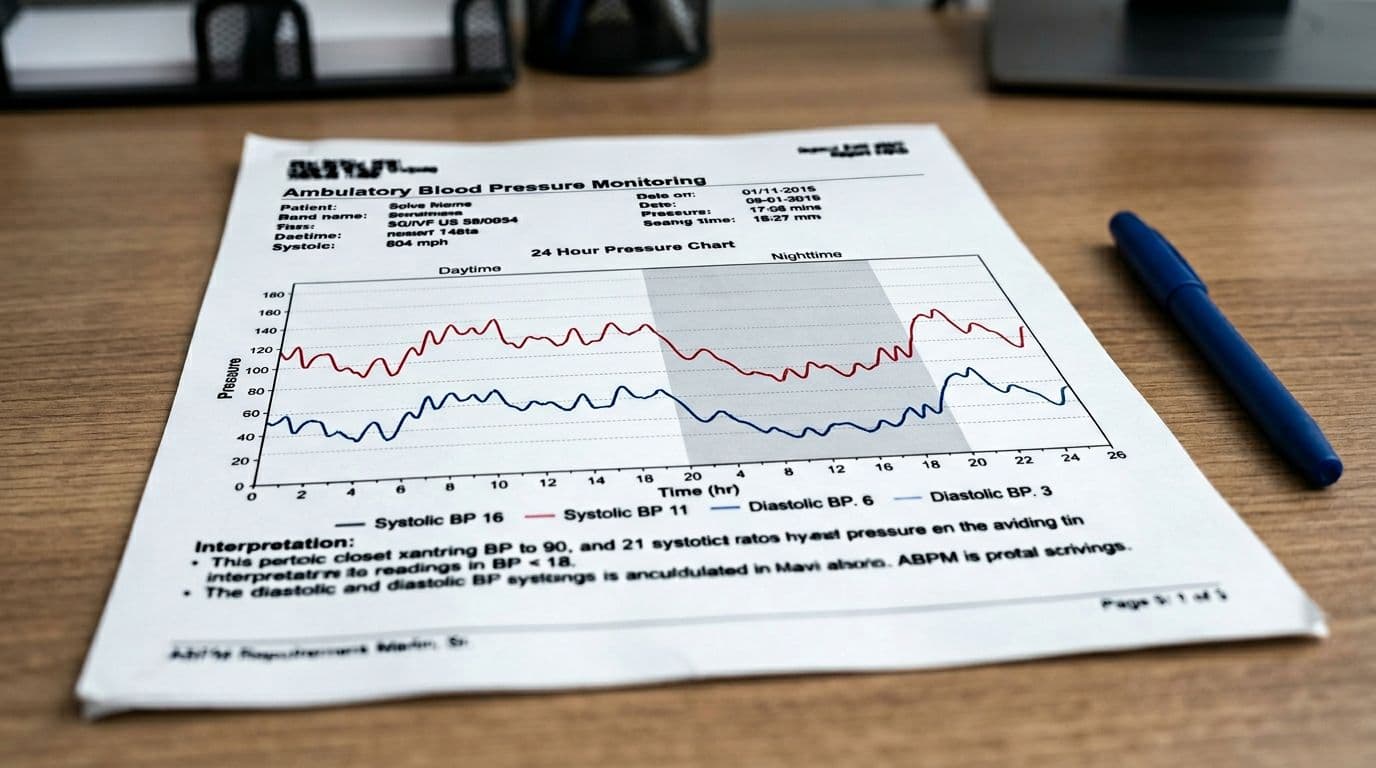
An ABPM report usually summarizes your average blood pressure across the full 24-hour period, then breaks it into daytime and nighttime periods. Think of it like a day-long weather report, not a single temperature reading.
Your clinician may look for blood pressure patterns such as average blood pressure that’s only high in the clinic (classic white coat pattern), average blood pressure that’s high outside the clinic (masked hypertension), or average blood pressure that doesn’t settle during sleep (nocturnal hypertension, a nighttime issue linked to increased cardiovascular risk).
A helpful way to frame ABPM is this: it doesn’t just answer “What’s my number?” It answers “What does my blood pressure do when my life happens?”
ABPM results can also shape treatment decisions. Real-world data sometimes shows fewer people truly need medication than office readings suggest. On the other hand, if ABPM confirms high ambulatory blood pressure, it can better predict future stroke and heart risk than a one-off office check.
When to ask your doctor for ambulatory blood pressure monitoring
ABPM isn’t for every situation, but it’s a smart ask when the stakes are high or the numbers don’t add up. Current guidance from the American Heart Association and European Society of Hypertension treats it as a standard of care medically necessary in several common scenarios, including confirming a new diagnosis, evaluating symptoms that might relate to low blood pressure, identifying resistant hypertension, and managing patients with chronic kidney disease.
Here’s a quick guide to help you decide whether to bring it up:
| Your situation | Why ABPM helps | What you might learn |
|---|---|---|
| Clinic readings are high, but home readings seem normal | Confirms or rules out white coat hypertension | Whether you can avoid unnecessary medication |
| Clinic readings are normal, but you feel “off” or your home readings run high | Detects masked hypertension | Whether your daily blood pressure is quietly high |
| You started or changed blood pressure medication and feel dizzy | Checks for hypotension during daily life | If dosing or timing needs adjustment |
| You have concerns about nighttime blood pressure | Sleep readings can reveal patterns | Whether nighttime pressure stays elevated |
| You suspect resistant hypertension (high BP despite multiple meds) | Confirms true resistant hypertension | If more evaluation or treatments are needed |
| You have chronic kidney disease | Provides accurate BP assessment in CKD patients | How to optimize management to protect kidneys |
Many clinicians avoid repeating ABPM too often. In practice, it’s often done for 24 hours, sometimes longer, and usually not repeated more than every 6 months unless there’s a clear reason. Medicare reimbursement is often available for specific indications like suspected white coat hypertension.
If you want to see how guideline updates have been discussed in plain language, this summary of an AHA/ACC blood pressure management guideline update offers helpful context. Also, this overview of how the American Heart Association updated high blood pressure guidance highlights how decision-making increasingly considers total heart risk, not just one number.
Using ABPM results to build a heart-smart routine that lasts
ABPM gives information, but your daily habits write the long story. A heart-healthy routine helps mitigate morning surges in blood pressure. Start with food and movement because they influence blood pressure, weight, sleep, and stress resilience. Tracking blood pressure readings at home can complement ABPM data to find a long-term average blood pressure.
A heart healthy diet doesn’t need perfection. It needs repeatable meals. Build your plate around healthy food you actually enjoy, then practice it until it’s automatic. For many people, a steady healthy food diet means more beans, vegetables, fruit, nuts, yogurt, olive oil, and fish, with fewer ultra-processed snacks and sugary drinks. That approach supports healthy nutrition and, over time, can support nutrition to prevent illness by lowering overall cardiometabolic strain.
Movement is the other half of the equation. Aim for a healthy living diet and exercise rhythm you can keep on your worst week, not just your best week. Brisk walking, cycling, swimming, and resistance training all count. If you want a practical plan, these strength training routines for heart health show how to lift without turning workouts into breath-holding battles.
Finally, remember that blood pressure is only one piece of heart risk. Some people do everything “right” and still carry extra inherited risk. If you’re thinking broadly about prevention, this guide on a Lipoprotein(a) test for heart risk assessment can help you understand another common, genetic risk factor that often pairs with blood pressure decisions.
That’s the spirit of sports and exercise for long life: not heroic bursts, but steady effort that keeps your arteries, muscles, and metabolism working together.
Conclusion: ask for the test when the story doesn’t match the snapshot
If your clinic readings and real life don’t agree, ambulatory blood pressure monitoring can bring clarity fast. It is the best tool for uncovering white coat hypertension, masked hypertension, and nighttime issues that a quick appointment can’t capture. Use the results as a map to reveal your blood pressure patterns, then follow the basics that still matter most: healthy nutrition, daily movement, sleep support, and a plan you can repeat. Rather than fixating on a single office number, focus on the blood pressure patterns of your daily life. What would your day-long “blood pressure weather report” reveal about your habits and stress?



0 Comments