Your legs can be strong, trained, and busy, yet the arteries feeding them might be quietly narrowing. Peripheral artery disease (PAD) often starts like that, no drama, just less blood getting through.
The ankle brachial index test (often shortened to ABI) is one of the simplest non-invasive procedures to spot that problem early. It’s quick, and it can connect the dots between leg symptoms and heart risk.
If you care about stamina, recovery, and a longer healthspan, ABI is worth understanding, because blood flow is the vital “supply chain” for every workout and every walk.
What the ankle brachial index test is really measuring (and why PAD matters)
Think of your arteries like a garden hose. When the hose is wide and clear, water moves freely. When plaque narrows the space, pressure and flow change, especially downstream.
The ankle brachial index test compares the systolic blood pressure at your ankle with the systolic blood pressure in your brachial artery. A Doppler ultrasound device helps measure ankle pressure accurately. If ankle pressure is much lower, it can suggest narrowed leg arteries, a hallmark of peripheral artery disease (PAD). Major medical centers describe ABI as a straightforward way to check for PAD and related cardiovascular risk, including the Mayo Clinic’s overview of the ankle-brachial index.
PAD is not just a “leg problem.” It is usually a sign of atherosclerosis elsewhere too. That is why a low ABI can raise concern about heart attack and stroke risk over time.
Symptoms can be obvious, but they can also be sneaky. Some people feel leg pain such as calf tightness or cramping while walking that eases with rest (claudication). Others just notice a slower pace, colder feet, or a sore that heals slowly. Athletic people sometimes chalk these signs up to aging or training fatigue, which delays answers.
PAD is more common when certain cardiovascular risk factors stack up, including smoking history, diabetes, high blood pressure, high cholesterol, kidney disease, and older age. If that sounds like your story, ABI is often a sensible next step to discuss with a clinician.
What happens during an ABI test appointment (and how to prep)
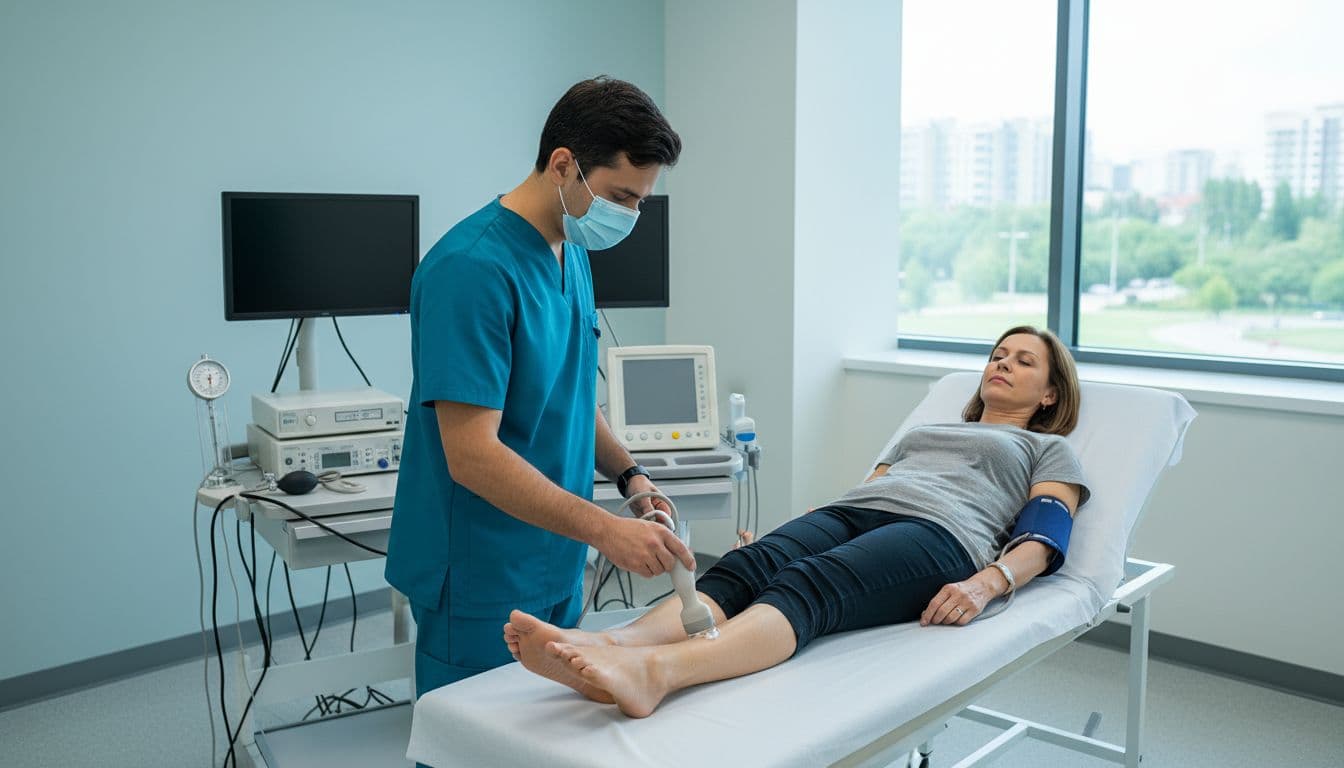
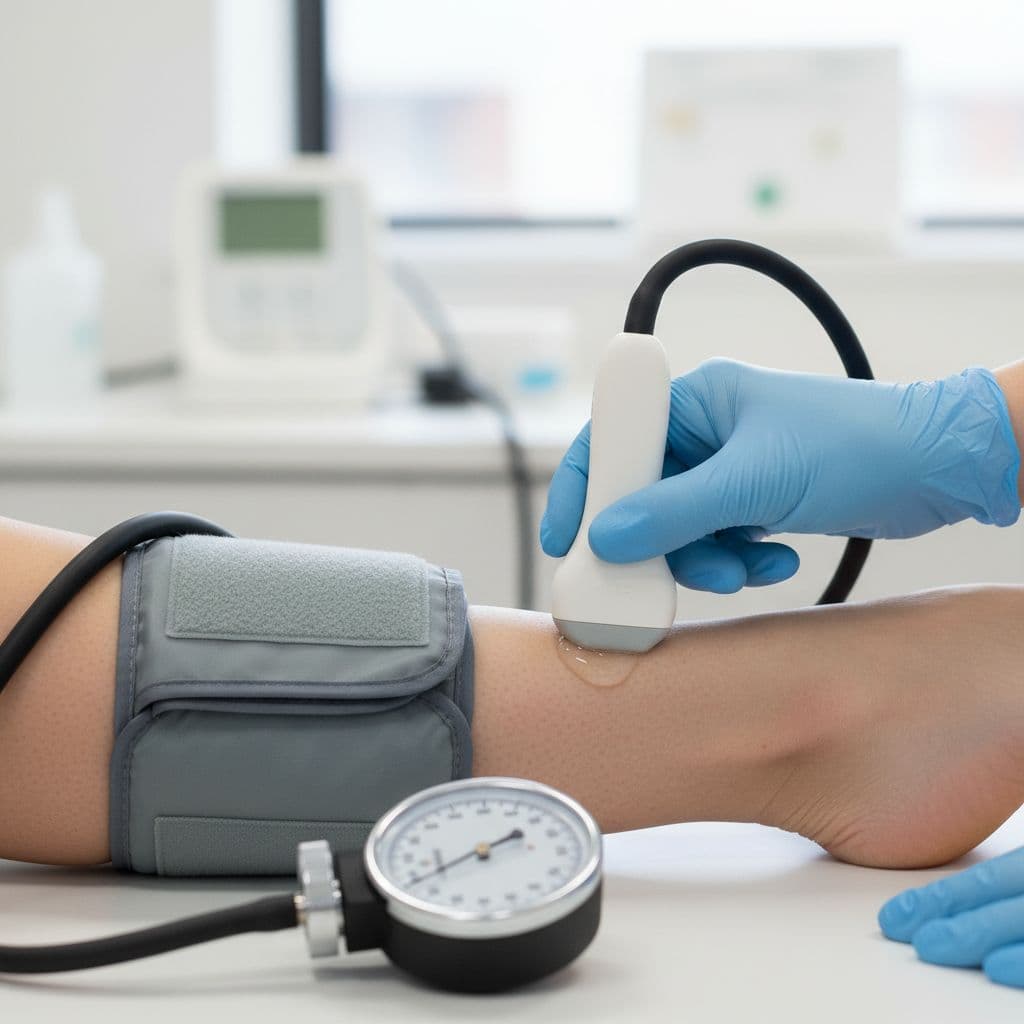
Most ABI tests take about 10 to 20 minutes. You’ll lie in a supine position and rest for several minutes first, because walking in from the parking lot can nudge numbers. Then a clinician places blood pressure cuffs on your upper arms over the brachial artery and ankles. Many clinics also apply ultrasound gel and use a handheld Doppler ultrasound device to listen for blood flow at the dorsalis pedis artery and posterior tibial artery while the blood pressure cuff pressure changes.
Here’s what you can do to make it smoother:
- Wear loose pants or shorts so the blood pressure cuffs can sit correctly.
- Skip hard exercise right before the visit if you can, ask the clinic for any special instructions.
- Tell the clinician about wounds, stents, or bypass surgery in your legs.
- Bring your medication list, especially blood pressure meds and blood thinners.
The test can feel tight, like any blood pressure cuff. Still, it shouldn’t be painful. If your legs cramp, you have leg pain, or you have nerve pain, say so early.
Some clinics add an “exercise ABI.” That means repeating the measurements after a treadmill exercise test to reveal blood flow limits that don’t show up at rest. If you want a simple patient-oriented walkthrough of what to expect, Newman Medical’s step-by-step ABI testing guide explains the common flow of an appointment.
How to read ABI results (normal, borderline, low, and “too high”)
To calculate ABI, divide the ankle pressure by the arm systolic blood pressure (measured for each leg):
Ankle systolic pressure ÷ Arm systolic blood pressure
Clinics may use slightly different cutoffs, but these ranges are widely used in practice and in reviews. The normal ABI range falls between 1.00 and 1.40:
| ABI value | What it can suggest | Common next step |
|---|---|---|
| > 1.40 | Stiff, calcified blood vessels (often with diabetes or kidney disease) | Consider toe-brachial index or vascular imaging |
| 1.00 to 1.40 | Within normal ABI range; usually normal blood flow | Maintain prevention habits |
| 0.91 to 0.99 | Borderline | Watch symptoms, manage risks, consider exercise ABI |
| 0.70 to 0.90 | Mild PAD | Lifestyle, meds, supervised exercise often recommended |
| 0.40 to 0.69 | Moderate PAD | Specialist evaluation, structured treatment plan |
| < 0.40 | Severe PAD (precursor to critical limb ischemia) | Prompt vascular specialist care to assess vascular status and wound healing |
A simple rule many clinicians use: ABI below 0.90 supports a PAD diagnosis, especially when symptoms match.
A “too high” ABI (over about 1.4) surprises people. It doesn’t mean superhuman arteries. It often means the artery walls are stiff due to calcified blood vessels, so the cuff can’t compress them well. In that case, especially with diabetes, clinicians may switch to a toe-brachial index, because toe arteries are less likely to be stiff.
If you’re wondering whether everyone should be screened, the U.S. Preventive Services Task Force states there isn’t enough evidence to recommend routine screening in adults without symptoms, summarized in its PAD screening recommendation using ABI. For deeper technical context, the NCBI Bookshelf systematic review for the USPSTF lays out what ABI can and can’t do in broad screening.
Lowering PAD risk: make blood flow a daily habit (food plus movement)
An ABI number is information, not a life sentence. If your result is borderline or low for peripheral artery disease, your daily choices can still shift the trajectory, especially when you start early.
Food comes first, because it shapes cholesterol, blood pressure, and blood sugar. A healthy food diet for artery support is less about perfect meals and more about repeatable defaults: beans, oats, vegetables, fruit, nuts, olive oil, and fish if you eat it. That’s the heartbeat of a heart healthy diet, and it supports healthy nutrition without turning dinner into a math problem, while promoting steady blood flow through nutrition-dense meals. For practical shopping and meal ideas, this guide to heart-healthy foods and simple meals fits real life.
Next, pair that with movement you can repeat. Walking is especially powerful for PAD, because it trains the legs to use oxygen better and can improve symptoms over time. Add strength training to keep muscle and balance as the years stack up. The goal is not punishment workouts, it’s sports and exercise for long life, the kind that still feels doable on a Tuesday.
Blood pressure matters too. Minerals like magnesium support normal vessel function, and many magnesium-rich choices also support fiber intake, which helps lipids. If you want a food-first approach, see these magnesium-rich foods for blood pressure.
Finally, remember the “big three” that protect arteries: don’t smoke, control diabetes if you have it, and treat high cholesterol when needed. For a clearer view of cholesterol-related risk beyond the basic panel, this breakdown of ApoB vs LDL for heart risk assessment can help you ask better questions.
This is healthy living diet and exercise in plain form: steady meals, steady movement, steady follow-up.
Conclusion
The ankle brachial index test is a critical tool for identifying PAD early, a simple pressure comparison that reveals a lot about leg arteries, blood flow, and long-term cardiovascular risk. If your ABI is low or unusually high, the next steps usually include more targeted testing and tighter risk-factor control. Most importantly, the everyday basics still matter: healthy food, consistent walking and strength work, and smart medical follow-up. Your arteries respond to what you repeat, so choose habits you can live with.



0 Comments